Relative risk: Providing critical context for a better understanding
What are absolute risk and relative risk?
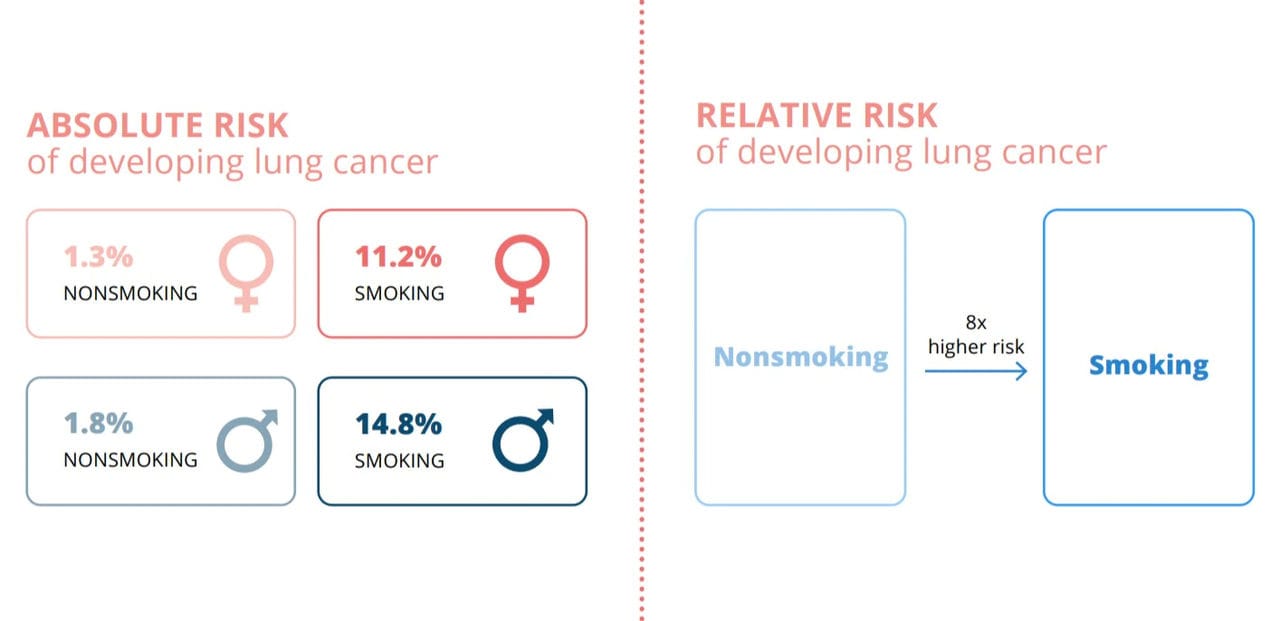
Adults who would otherwise continue to smoke should have access to accurate information about scientifically substantiated, less harmful alternatives that the advance in science and technology may make available to them. Understanding the difference between relative and absolute risk is key when looking at harm reduction for smokers. Relative risk compares the risk between certain groups. For instance, stated in terms of relative risk, a 2021 study by Bruder et al. estimated that a smoker is around eight times more likely to develop lung cancer than a nonsmoker. However, in absolute risk terms, a woman who smokes has an 11.2% (14.8% for men) risk of developing lung cancer, versus a nonsmoking woman’s 1.3% risk (1.8% for men).

In scientific terms, absolute risk is the number of people experiencing an event in relation to the population at risk – often presented as a percentage or as a ratio, like “1 in 10 people.” Relative risk is often communicated in a similar way, but with key words added to indicate that a comparison is being made, such as “10% higher/lower risk” or “five times more/less likely to…” Relative risk information can promote understanding of the implications of absolute risk by providing the context for how specific factors or behaviors, such as age, sex, physical activity, and diet, are estimated to impact our chances, for example, of developing a disease or health issue.
Both methods of communicating risk can provide important information when they’re based on scientific facts, and both have their place in scientific discussion. Relative risk communications can be more impactful because they provide context for the reader, but they’re also a bit more complex as they convey more information at once. Relative risk statements need to use the right comparator to properly convey an understanding of the estimate. When talking about tobacco harm reduction, we could consider comparing the estimated risks of a product to those estimated for cessation, continued smoking, never smoking, and even other products. What makes the most sense to best communicate about these products’ risk profiles?
Not all tobacco products are equal
The best way to minimize one’s risk of smoking-related diseases, including lung cancer, chronic obstructive pulmonary disease (COPD) and cardiovascular diseases, is to never start smoking at all. For current smokers (about 1 billion people globally), the best single step they can take to reduce their risk of harm is to quit tobacco and nicotine use altogether. The more people who do this, the bigger the reduction in population harm that is caused by smoking cigarettes. For adult smokers who would otherwise continue smoking, switching to scientifically substantiated smoke-free alternatives has the potential to reduce their risk of developing major smoking-related diseases. However, these products are not risk free and contain nicotine, which is addictive.
Reducing tobacco-related harm at the population level through less harmful alternatives, depends not only on the absolute risk to the individual using the product, but also its adoption by adult smokers. The biggest impact on population health occurs when as many smokers as possible quit altogether or if adults who would otherwise continue to smoke switch to scientifically substantiated lower risk products, rather than continuing to smoke cigarettes. Not all tobacco products are the same. Their use exists along a continuum of risk, where smoking combusted tobacco yields the highest risk and quitting nicotine and tobacco products altogether contributes the lowest risk. The use of other tobacco products, including smoke-free products, also lie in that continuum of risk. Products that don’t burn tobacco are likely to be far less harmful alternatives to continued smoking.
A study, for example, indicated that emissions from vaporized nicotine (e.g., e-cigarettes) and HTPs, contain carcinogens but generally in lower concentrations than found in cigarette smoke. Both product categories had more than an order of magnitude lower cancer potency than cigarettes according to the study’s criteria. When it comes to risk of harm, it’s smokers switching completely that is important, not which lower risk product they switch to.

Why is relative risk is important
Switching from cigarettes to a nicotine-containing product that is avoiding combustion carries a higher risk than either abstinence or cessation, which remain the absolute best choice one can make. That is why smoke-free products are developed for and marketed to adults who would otherwise continue to smoke cigarettes, and not to youth, nonsmokers or former smokers. Adults who smoke are aware of the risks of smoking, and so learning that there are other products whose risks may be lower than that of continued cigarette smoking could encourage them to switch.
This is why it is so important to include comparisons between the use of smoke-free products and cigarettes in scientific studies. The aim is to build scientific evidence that will demonstrate the likely reduced-risk profile of smokers who completely switch to smoke-free products. Other comparisons can still be informative, but leaving out this comparison means we miss out on critical context for our results. The goal is to determine if the risk profile of switching to a smoke-free product is similar to continued smoking, or to smoking cessation, or somewhere in between.
The harm reduction equation
Now, reducing the risk of harm for an individual is not enough to reduce the risk of harm for an entire population. The more individuals who choose the lowest risk options instead of continuing to smoke, the bigger the impact on reducing population harm. This is known as the harm reduction equation.


Read the Scientific Update magazine
The Scientific Update magazine is focused on PMI's research and development efforts, milestone studies, industry regulations, and more. View the latest issue, or read the articles online.


